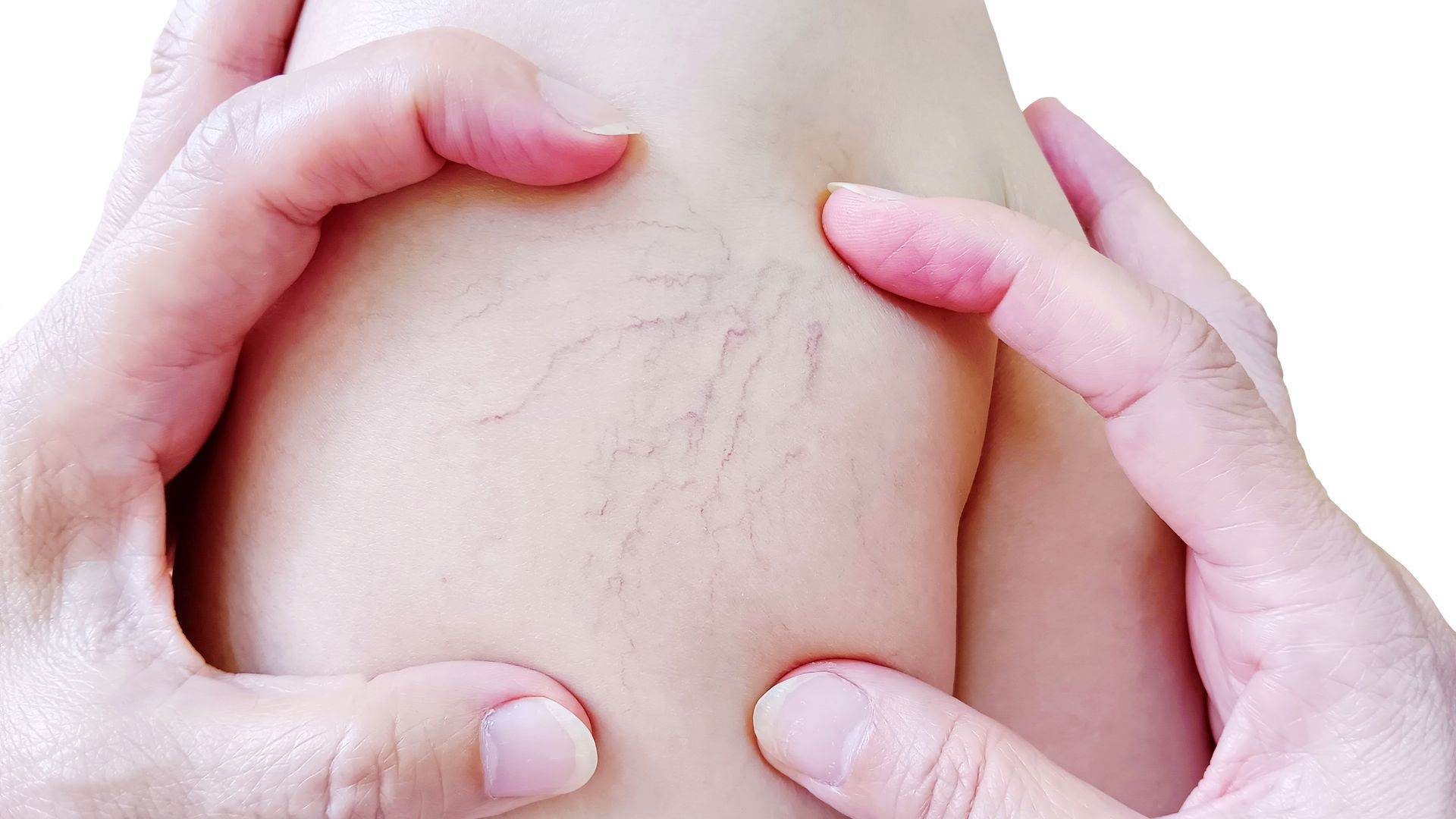
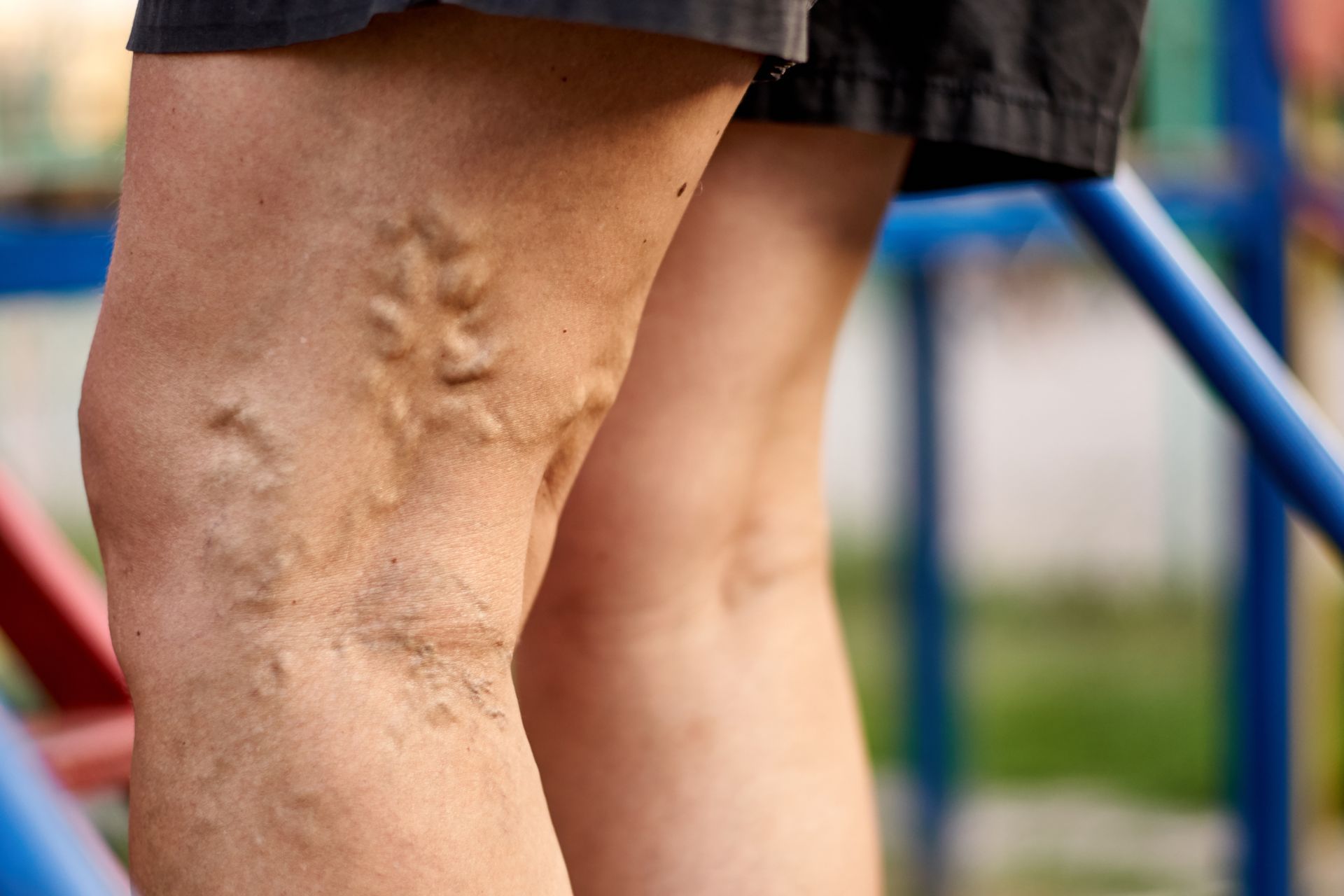
Can PAD Be Reversed? Treatment Options Explained
Key Points
- PAD cannot be completely "cured," but symptoms can significantly improve and disease progression can be slowed or stopped
- Lifestyle changes and medications form the foundation of effective PAD treatment
- Minimally invasive procedures can restore blood flow and dramatically reduce symptoms
- Early treatment offers the best chance for improvement and prevents serious complications
- The right treatment plan depends on your PAD severity, overall health, and personal goals
- Ascent Vascular offers comprehensive PAD treatment from conservative management to advanced procedures
The Question Every PAD Patient Asks
If you've been diagnosed with peripheral arterial disease, you've probably wondered: can this be fixed? Can my arteries go back to normal? Will I always have to deal with leg pain when I walk?
These are the questions we hear every day at Ascent Vascular. And while we wish we could say there's a magic cure that makes PAD disappear completely, the reality is more nuanced and, honestly, more hopeful than you might think.
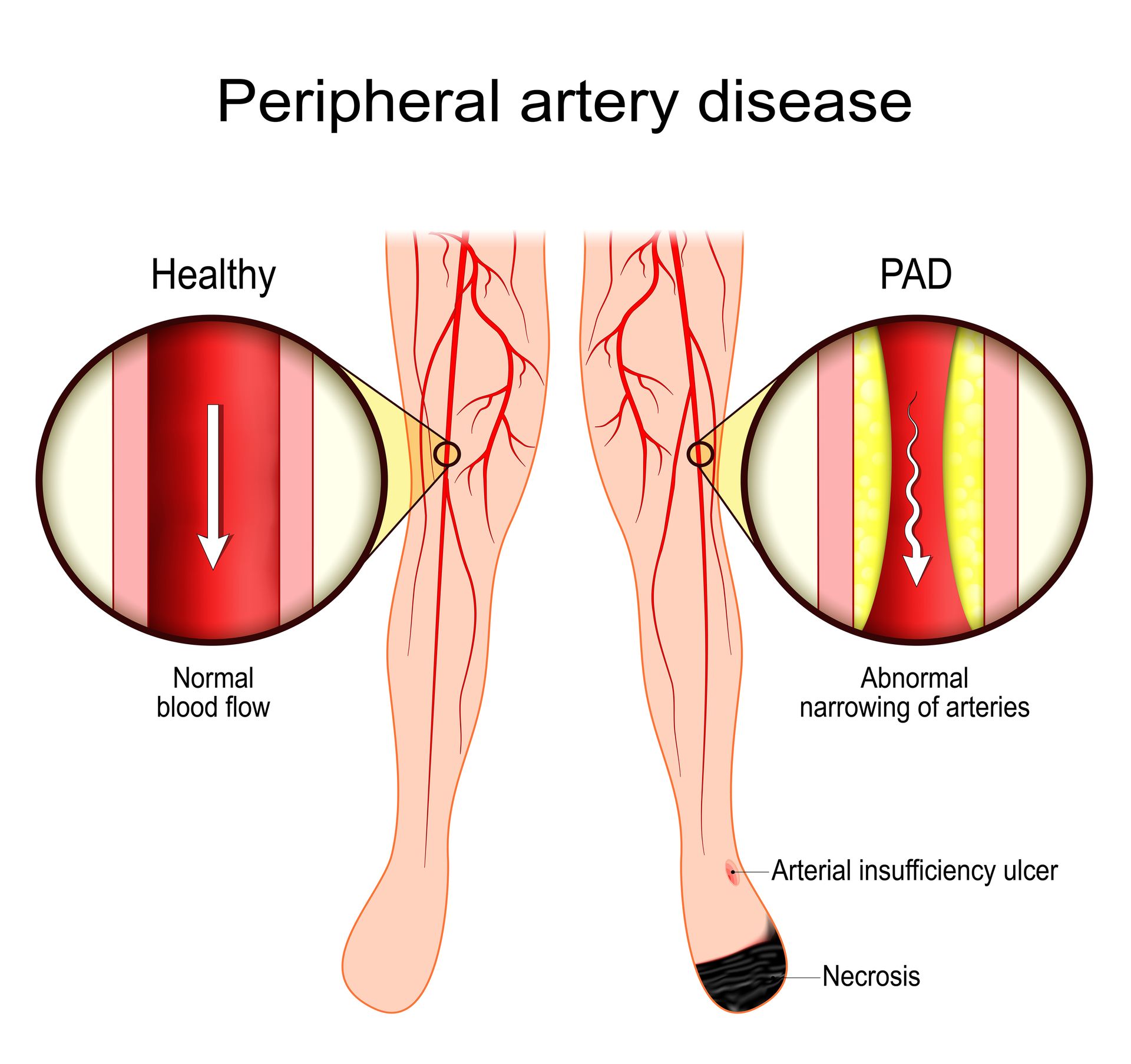
Here's the straight answer: PAD cannot be completely reversed in the sense of making your arteries look like they did when you were 20. The plaque buildup that's narrowed your arteries can't be entirely eliminated. However, and this is the important part, PAD can absolutely be treated, managed, and in many cases dramatically improved. Many people see significant symptom relief, increased walking distance, and better quality of life with the right treatment approach.
Think of it less like reversing and more like remodeling. We might not be able to restore your original plumbing, but we can definitely improve the flow, reduce your symptoms, prevent the problem from getting worse, and help you get back to doing the things you love.
Understanding What Treatment Can and Cannot Do
Let's set realistic expectations from the start. Understanding what's possible helps you make informed decisions about your care and stay motivated with your treatment plan.
What PAD Treatment CAN Do
Significantly improve symptoms. Many people experience substantial reduction in leg pain and cramping with proper treatment. Some see their claudication (walking pain) decrease dramatically or even disappear.
Increase walking distance. Treatment, especially combined lifestyle changes and medical interventions, can help you walk farther before experiencing discomfort.
Restore blood flow. Procedures like angioplasty and stenting can open blocked arteries and restore more normal circulation to your legs.
Prevent progression. Aggressive risk factor management can stop PAD from getting worse and protect you from developing critical limb ischemia.
Reduce heart attack and stroke risk. Since PAD indicates you likely have plaque buildup elsewhere, treating PAD and its underlying causes protects your overall cardiovascular health.
Heal ulcers and wounds. Improved blood flow allows slow-healing or non-healing wounds to finally close.
Prevent amputation. Early and effective treatment dramatically reduces the risk of losing a limb to PAD.
Improve quality of life. Better circulation means more energy, less pain, greater mobility, and the ability to stay active and independent.
What PAD Treatment CANNOT Do
Completely remove all plaque. The atherosclerosis (plaque buildup) that caused your PAD developed over years or decades. We can't make it vanish entirely.
Guarantee you'll never have symptoms again. Even with successful treatment, you'll need ongoing management and might still have some limitations.
Replace the need for lifestyle changes. Even the best procedures work better and last longer when combined with healthy habits like not smoking, eating well, and staying active.
Work instantly. Most treatments take time to show full benefits. Patience and consistency matter.
The good news? For most people with PAD, significant improvement is absolutely achievable. Let's look at how.
The Foundation: Lifestyle Changes and Medications
Before we dive into procedures, it's crucial to understand that the foundation of PAD treatment is managing risk factors and optimizing your overall vascular health. For many people with mild to moderate PAD, this conservative approach provides substantial relief.
Lifestyle Modifications That Make a Real Difference
Quitting smoking is non-negotiable. If you smoke, this single change has more impact than anything else you can do. Smoking accelerates PAD progression, worsens symptoms, and dramatically increases your risk of amputation. Within weeks of quitting, your circulation starts improving.
Starting a walking program might seem counterintuitive when walking causes pain, but it's one of the most effective treatments for claudication. Regular walking to the point of mild discomfort, followed by rest, actually helps your body develop new small blood vessels that bypass blockages. Over time, many people can walk significantly farther with less pain. You can learn more about implementing an effective walking routine in our daily PAD management guide.
Adopting a heart-healthy diet helps slow plaque buildup. Focus on fruits, vegetables, whole grains, lean proteins, and healthy fats while limiting saturated fat, trans fat, and excess sodium. These dietary changes help control cholesterol, blood pressure, and blood sugar, all of which affect PAD progression.
Managing diabetes, high blood pressure, and high cholesterol aggressively protects your blood vessels from further damage. Keeping these conditions well-controlled is essential for preventing PAD from worsening.
Maintaining a healthy weight reduces strain on your circulatory system and helps control other risk factors.
You can explore more about how healthy habits prevent and manage vascular problems on our blog.
Medications for PAD
Most people with PAD benefit from medications, even if they're also having procedures. Common medications include:
Antiplatelet drugs like aspirin or clopidogrel (Plavix) prevent blood clots and reduce your risk of heart attack and stroke. These are often prescribed for life.
Cholesterol-lowering medications, especially statins, do more than just lower cholesterol. They stabilize existing plaque, reduce inflammation in blood vessels, and slow disease progression. Many people with PAD benefit from statins even if their cholesterol seems acceptable.
Blood pressure medications protect your arteries from damage and reduce cardiovascular risk.
Cilostazol is specifically approved for claudication. It improves blood flow and can help some people walk farther before experiencing pain. Not everyone can take this medication, but when appropriate, it can be quite helpful.
Diabetes medications if you have diabetes, maintaining good blood sugar control is crucial.
Think of medications as part of your long-term management strategy, working behind the scenes to protect your vascular system and prevent complications.
When Lifestyle and Medications Aren't Enough
For some people, conservative treatment provides excellent symptom control. For others, symptoms persist or worsen despite best efforts with lifestyle changes and medications. That's when more invasive interventions become appropriate.
Signs You Might Need a Procedure
Your doctor might recommend a procedure if you have:
- Severe claudication that significantly limits your daily activities despite conservative treatment
- Rest pain (pain in your legs or feet when you're not active, especially at night)
- Non-healing wounds or ulcers on your feet or legs
- Signs of critical limb ischemia
- Significant blockages found on imaging tests
The goal isn't to jump to procedures unnecessarily, but rather to use them strategically when they'll meaningfully improve your quality of life or prevent serious complications.
Minimally Invasive Treatments for PAD
Modern vascular medicine has come a long way. Many PAD treatments that once required major surgery can now be done with minimally invasive techniques. These procedures typically involve small incisions, local anesthesia or light sedation, and quick recovery times.
Angioplasty and Stenting
This is one of the most common treatments for PAD and works remarkably well for many patients.
How it works: Your doctor threads a thin catheter through a small incision (usually in your groin or arm) and guides it to the blocked artery using X-ray imaging. A tiny balloon at the catheter's tip is inflated inside the blocked area, compressing the plaque against the artery wall and widening the opening. Often, a small mesh tube called a stent is placed to keep the artery open.
What it treats: Angioplasty works best for discrete blockages in larger arteries. It's particularly effective for blockages in the iliac arteries (in your pelvis) and femoral arteries (in your thigh).
The procedure experience: Most angioplasties are outpatient procedures. You'll be awake but sedated and won't feel pain. The procedure typically takes 1-3 hours. You'll need to lie flat for several hours afterward to prevent bleeding from the catheter insertion site, then you can usually go home the same day.
Recovery: Most people return to normal activities within a few days. You'll take blood thinners to prevent clots around the stent.
Success rates: Many people experience immediate improvement in symptoms. Stents in larger arteries (like the iliac arteries) tend to stay open long-term. Smaller arteries have somewhat higher rates of re-narrowing, but repeat procedures can be done if needed.
Atherectomy
For some types of blockages, especially heavily calcified plaque, atherectomy might be used instead of or in addition to angioplasty.
How it works: A specialized catheter with a tiny rotating blade or laser shaves away or vaporizes plaque from the artery wall. The debris is collected and removed.
What it treats: Atherectomy is particularly useful for very hard, calcified blockages that might not respond well to balloon angioplasty alone.
The procedure: Similar to angioplasty in terms of technique and recovery. It's often combined with balloon angioplasty for optimal results.
Bypass Surgery
While less common than it used to be, bypass surgery is still sometimes the best option for certain PAD cases.
How it works: A surgeon creates a detour around the blocked artery using either a vein from your leg or a synthetic graft. Blood flows through this new pathway, bypassing the blockage entirely.
What it treats: Bypass is typically reserved for extensive blockages, blockages in locations not suitable for angioplasty, or cases where angioplasty has failed. It's also used for critical limb ischemia when saving the limb is at stake.
The procedure: This is actual surgery requiring general anesthesia and a hospital stay of several days. Recovery takes longer than minimally invasive procedures, usually several weeks.
Success rates: When performed for appropriate cases, bypass grafts can remain open and functioning for many years.
Emerging and Advanced Therapies
Vascular medicine continues evolving. While not yet mainstream, several newer approaches show promise:
Drug-coated balloons and stents release medication directly to the artery wall to prevent re-narrowing. These are becoming more common and showing good results in some cases.
Gene therapy and stem cell treatments are being studied as ways to stimulate new blood vessel growth. While still largely experimental, research is ongoing.
At Ascent Vascular, we stay current with the latest evidence-based treatments and can discuss whether newer approaches might be appropriate for your situation.
Emerging and Advanced Therapies
Vascular medicine continues evolving. While not yet mainstream, several newer approaches show promise:
Drug-coated balloons and stents release medication directly to the artery wall to prevent re-narrowing. These are becoming more common and showing good results in some cases.
Gene therapy and stem cell treatments are being studied as ways to stimulate new blood vessel growth. While still largely experimental, research is ongoing.
At Ascent Vascular, we stay current with the latest evidence-based treatments and can discuss whether newer approaches might be appropriate for your situation.
Choosing the Right Treatment for You
There's no one-size-fits-all approach to PAD treatment. The best plan depends on multiple factors:
Your PAD severity: Mild disease might respond well to lifestyle changes alone, while severe disease might require procedures.
Location and extent of blockages: Some blockages are easier to treat with minimally invasive techniques than others.
Your overall health: Other medical conditions affect which treatments are safest and most appropriate for you.
Your symptoms and how they affect your life: Two people with similar blockages might make different treatment choices based on their activity goals and symptom tolerance.
Your preferences and goals: Some people prefer starting with the most conservative approach and progressing only if needed. Others want more aggressive intervention upfront to maximize symptom relief.
When you visit our team at Ascent Vascular, we'll discuss all these factors and create a personalized treatment plan that aligns with your goals and gives you the best chance for improvement.
What to Expect After Treatment
Regardless of which treatment you pursue, success requires ongoing commitment.
Immediate Results
Many people notice improvement quickly after procedures like angioplasty. Leg pain might decrease significantly or disappear, walking distance often increases, and wounds may begin healing. However, full benefits sometimes take weeks or months to manifest.
Conservative treatments like walking programs and medications work more gradually. You might not notice dramatic changes week to week, but over months, improvement can be substantial.
Long-Term Success Requires Maintenance
Here's the critical part: no PAD treatment works in isolation. Even after a successful procedure, you still need to:
Continue lifestyle modifications. Quitting smoking, exercising regularly, and eating healthfully aren't just for before treatment. They're lifelong commitments that help maintain results.
Take medications as prescribed. Blood thinners, statins, and other medications protect your treated arteries and prevent new blockages.
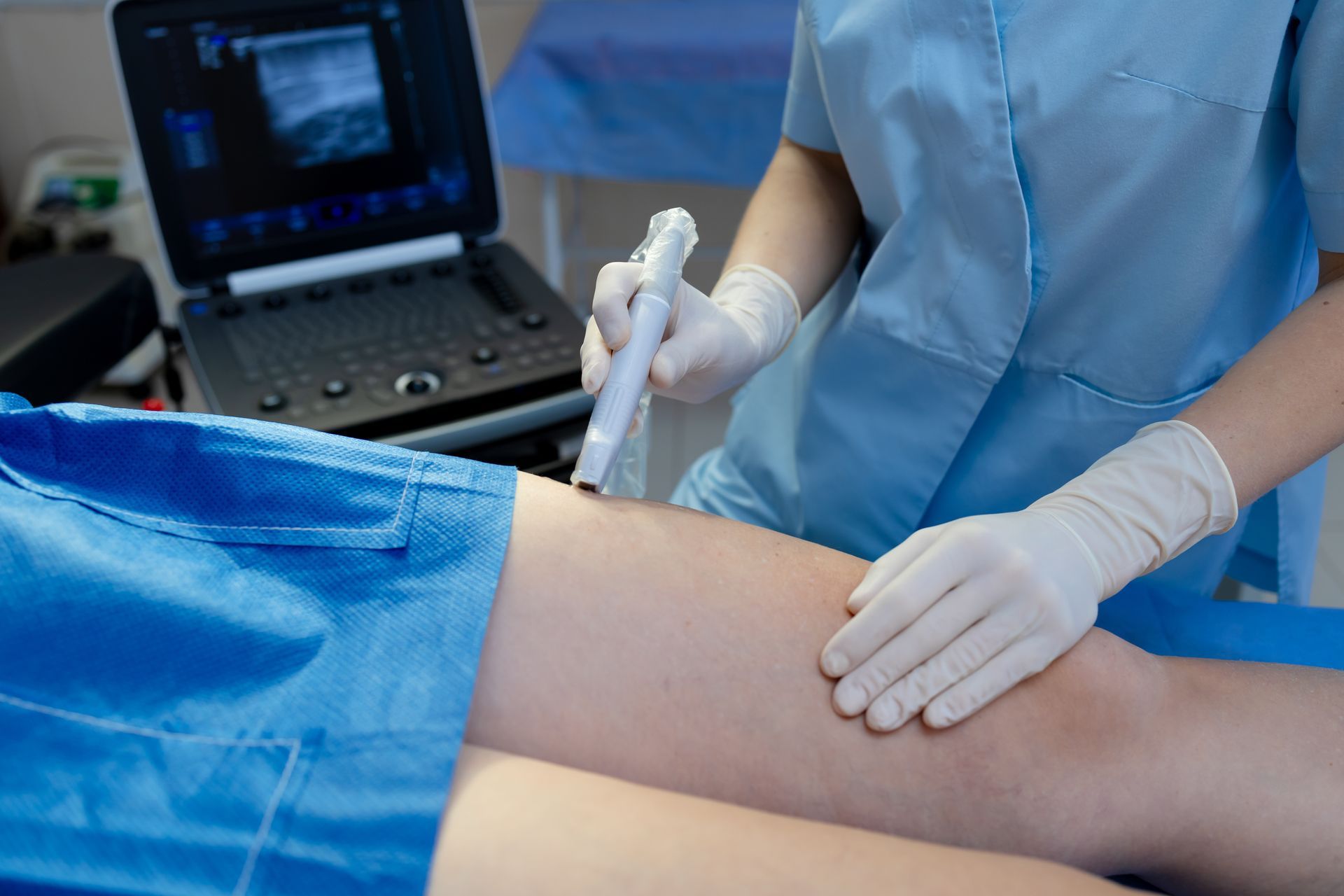
Attend follow-up appointments. Regular monitoring with your vascular specialist helps catch any problems early. We'll use tests like vascular ultrasound to check on treated areas.
Stay vigilant about symptoms. Report any return or worsening of symptoms promptly. Sometimes treated arteries can narrow again, and early intervention prevents serious problems.
Think of PAD treatment as starting a new chapter, not closing the book. The tools we provide through procedures and medications work best when you continue doing your part with healthy habits.
The Reality of Re-Blockage
It's important to discuss this honestly: treated arteries can sometimes narrow again. This is called restenosis, and it happens in a percentage of cases, especially in smaller arteries below the knee.
Why it happens: Your body's healing response to the procedure can sometimes cause scar tissue formation that narrows the artery. Also, the underlying disease process (atherosclerosis) that caused PAD doesn't disappear just because one area was treated.
How common it is: Rates vary depending on the location treated, type of procedure, and how well you manage risk factors afterward. Larger arteries like the iliac arteries tend to stay open better than smaller ones. Using drug-coated devices can reduce restenosis rates.
What happens if it occurs: The good news is that re-blockage can often be treated with repeat procedures. Many people have angioplasty more than once over the years and continue doing well.
How to minimize risk: Aggressive risk factor management, taking medications as prescribed, and not smoking are the best ways to keep treated arteries open long-term.
Prevention Is Still the Best Medicine
While we're discussing treatment, it's worth emphasizing that preventing PAD progression is just as important as treating existing disease.
If you have PAD, you're at higher risk for developing blockages in other arteries, including those supplying your heart and brain. The same aggressive management that helps your leg arteries also protects against heart attack and stroke.
This is why your vascular specialist cares so much about your cholesterol levels, blood pressure, diabetes control, and especially smoking status. We're not just treating your legs; we're protecting your entire cardiovascular system.
Success Stories: What Improvement Really Looks Like
We've treated many PAD patients over the years, and while everyone's journey is unique, certain patterns emerge:
The motivated lifestyle modifier: This person commits fully to quitting smoking, walking daily, and eating better. Over six months, their claudication improves significantly. They're walking twice as far as when diagnosed and feeling more energetic overall. They've avoided procedures entirely through dedicated lifestyle management.
The angioplasty success: This person had severe claudication limiting them to walking less than a block. After angioplasty and stenting of a blockage in the femoral artery, combined with medication and a walking program, they're back to hiking Colorado trails with minimal discomfort. They maintain results through continued healthy habits and regular follow-up.
The complex case: This person had multiple blockages and tried conservative treatment first. When symptoms progressed to rest pain, they had a combination of procedures over time. While not "cured," they're pain-free, active, and their leg is healthy. They manage their condition with ongoing medical care and lifestyle modifications.
These examples illustrate an important point: success isn't always about being symptom-free or having "perfect" arteries. Success is about improving your quality of life, preventing serious complications, and maintaining your independence and activity level.
The Bottom Line on PAD Reversal
So, can PAD be reversed? Here's the honest answer:
PAD is a chronic condition resulting from years of plaque buildup in your arteries. That plaque can't be magically erased. However, PAD absolutely can be treated, managed, and improved. Many people with PAD experience dramatic symptom relief, return to activities they love, and prevent the disease from progressing.
The key is thinking of PAD treatment as a comprehensive, ongoing approach rather than a one-time fix. Combining lifestyle changes, medications, and procedures when appropriate gives you the best chance for improvement and long-term success.
Early treatment offers the best outcomes. The longer PAD goes untreated, the more difficult it becomes to manage and the higher the risk of serious complications.
If you've been diagnosed with PAD, or if you're experiencing symptoms like leg pain when walking, don't wait to seek help. Modern treatments can make a real difference, but only if you take that first step.
FAQs About PAD Treatment and Reversal
How long does it take to see improvement from PAD treatment?
This varies by treatment type. After angioplasty or stenting, some people notice improvement within days. With conservative treatments like walking programs and medications, meaningful improvement typically takes 3-6 months of consistent effort. Be patient and stick with your treatment plan even if changes seem slow at first.
Will insurance cover PAD treatment?
Most insurance plans, including Medicare, cover medically necessary PAD treatment. Coverage includes diagnostic tests, medications, and procedures when appropriate. We recommend checking with your insurance provider about specific coverage, and our team can help verify benefits before treatment.
Can PAD come back after successful treatment?
Treated arteries can sometimes narrow again (restenosis), and new blockages can develop in other arteries. This is why ongoing risk factor management and lifestyle modifications are so important even after successful procedures. Regular follow-up helps catch problems early if they occur.
Is one treatment better than another for PAD?
There's no single "best" treatment for everyone. The most appropriate approach depends on your specific blockage locations, PAD severity, overall health, and personal goals. For mild to moderate PAD, conservative treatment is usually tried first. For severe symptoms or critical limb ischemia, procedures are often necessary. Your vascular specialist will recommend the best approach for your situation.
What happens if I don't treat my PAD?
Untreated PAD often progresses over time. Symptoms typically worsen, walking becomes more difficult, and the risk of serious complications increases. These complications can include critical limb ischemia, non-healing wounds, infections, and in severe cases, amputation. PAD also indicates increased risk for heart attack and stroke. Early treatment prevents these outcomes.
What should I do if I develop a blister or cut on my foot?
Clean it gently with mild soap and water, apply antibiotic ointment if recommended by your doctor, and cover it with a clean bandage. Monitor it closely for signs of infection (increasing redness, warmth, swelling, drainage, or red streaks). Contact your doctor right away if it's not healing or shows signs of infection. Don't wait.
Can I ever stop taking medications if my PAD improves?
Many people with PAD continue working successfully. However, jobs requiring prolonged standing or walking might need modifications. Talk to your employer about accommodations like sitting breaks, job restructuring, or assistive devices if needed. Your doctor can provide documentation if necessary.
Will my PAD keep getting worse no matter what I do?
Even if your symptoms improve significantly, you'll likely need to continue medications long-term. These medications don't just treat symptoms; they prevent disease progression and protect you from cardiovascular events. Never stop medications without discussing it with your doctor first.
How do I know if I need a procedure or if lifestyle changes are enough?
Your vascular specialist will help make this determination based on your symptoms, how much they limit your daily life, how well conservative treatment is working, and what diagnostic tests show. Generally, if lifestyle changes and medications adequately control symptoms, procedures aren't necessary. If symptoms are severe, worsening, or conservative treatment isn't helping after a reasonable trial period, procedures become appropriate.
Are PAD procedures painful?
Most minimally invasive procedures are done with sedation and local anesthesia, so you won't feel pain during the procedure. Afterward, you might have some soreness at the catheter insertion site, but this is usually mild and managed easily with over-the-counter pain medication. Most people find the procedures much less uncomfortable than they anticipated.
FAQs About Ascent Vascular Specialist and Vein Center
What PAD treatments does Ascent Vascular offer?
We provide comprehensive PAD care including diagnostic testing, medication management, lifestyle counseling, and minimally invasive procedures like angioplasty and stenting. We'll evaluate your specific situation and recommend the most appropriate treatment approach for you.
How do I know if I'm a candidate for minimally invasive PAD treatment?
The best way to find out is through an evaluation with our vascular specialist. We'll review your symptoms, medical history, and perform diagnostic tests to determine which treatments are most appropriate for your situation. Contact us to schedule a consultation.
Do you perform PAD procedures in-office or at a hospital?
This depends on the specific procedure and your overall health. Many minimally invasive procedures can be done in outpatient settings. We'll discuss the details when developing your treatment plan.
How long is recovery after a PAD procedure?
For minimally invasive procedures like angioplasty, most people go home the same day and return to normal activities within a few days. Recovery from bypass surgery takes longer, typically several weeks. We'll give you specific recovery guidelines based on your procedure.
Will I need ongoing monitoring after PAD treatment?
Yes, regular follow-up is important to ensure treatments are working, check that arteries remain open, and monitor your overall vascular health. We'll create a follow-up schedule tailored to your needs, which typically includes periodic visits and imaging tests.
Can you help me quit smoking as part of my PAD treatment?
Absolutely. Smoking cessation is such a critical part of PAD treatment that we make it a priority in your care plan. We can provide resources, connect you with smoking cessation programs, and discuss medications that might help you quit successfully.
Take Control of Your PAD Today
Living with peripheral arterial disease doesn't mean accepting a life of pain and limitations. While PAD can't be completely "reversed," it can absolutely be treated, managed, and improved. The right combination of lifestyle changes, medications, and procedures when appropriate can help you regain mobility, reduce symptoms, and protect your overall health.
The most important step is getting started. Every day you wait is a day your PAD could be progressing. Early intervention offers the best chance for improvement and prevents serious complications.
At Ascent Vascular Specialist and Vein Center, we specialize in comprehensive PAD care. From initial diagnosis to ongoing management, we're here to help you achieve the best possible outcomes. Our Edwards, Colorado location serves patients throughout the Vail Valley with state-of-the-art diagnostic technology and proven treatment methods.
Ready to explore your PAD treatment options? Contact us today to schedule a consultation, or call our office at (970) 926-1003. Let's discuss what's possible for your specific situation and develop a treatment plan that helps you get back to living life on your terms.
Visit us at: Ascent Vascular Specialist and Vein Center 1140 Edwards Village Blvd. B204 Edwards, CO 81632
You can also learn more about peripheral arterial disease and other vascular conditions we treat, explore our available treatments, or read more about your vascular health on our blog.
Disclaimer: The information provided on this blog is for general informational purposes only and is not intended as, and should not be considered, medical advice. All information, content, and material available on this blog are for general informational purposes only. Readers are advised to consult with a qualified healthcare professional for medical advice, diagnosis, or treatment. The author and the blog disclaim any liability for the decisions you make based on the information provided. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.