Living with PAD: Daily Management Tips and Lifestyle Adjustments
Key Points
- PAD requires daily attention, but you can maintain an active, fulfilling life with the right strategies
- A structured walking program is the single most effective lifestyle intervention for PAD symptoms
- Daily foot checks and proper foot care prevent serious complications
- Small lifestyle adjustments like eating heart-healthy foods and quitting smoking slow disease progression
- Regular symptom monitoring helps you recognize when to seek medical attention
- Ascent Vascular provides ongoing support and personalized management plans for PAD patients
You Can Live Well with PAD
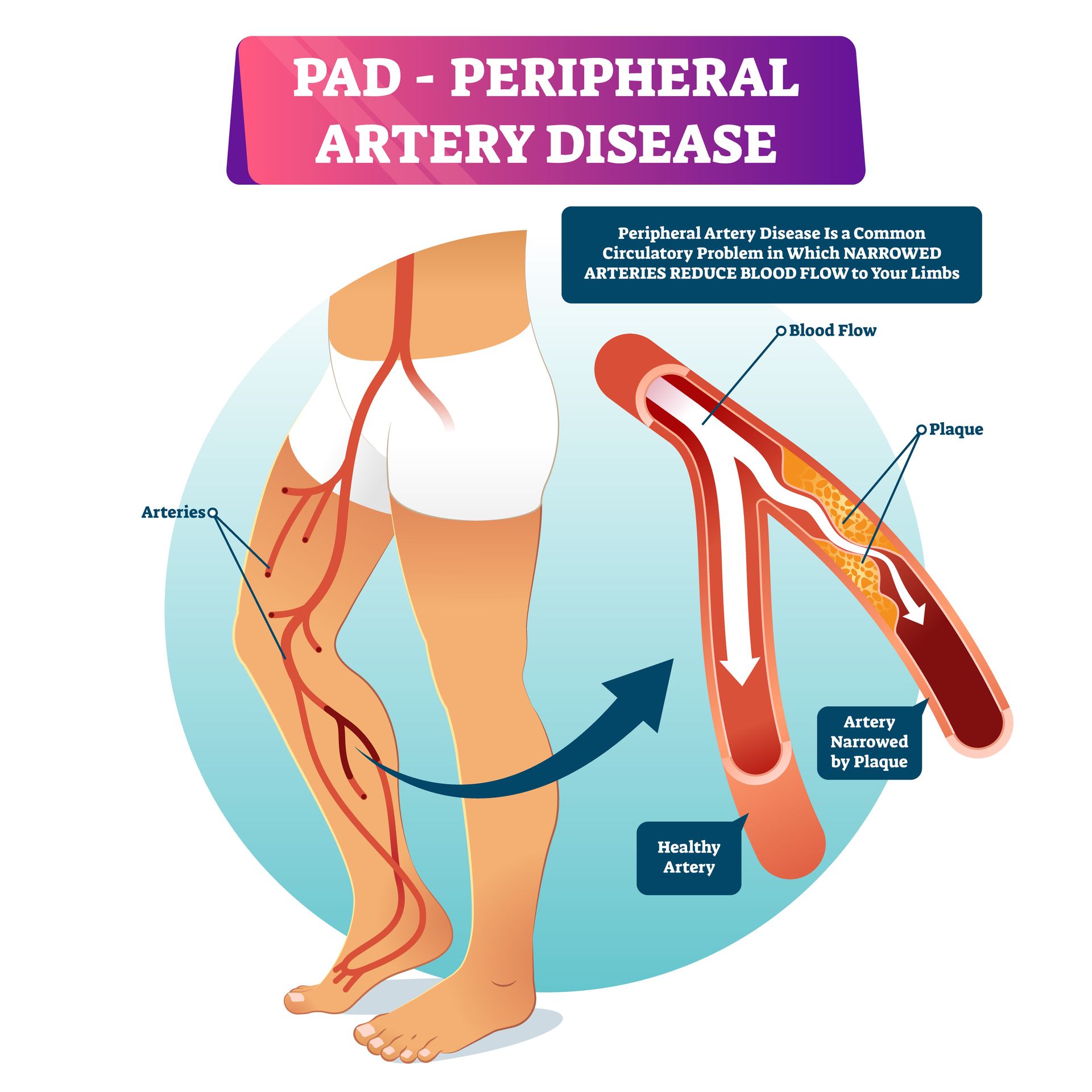
Getting diagnosed with peripheral arterial disease can feel overwhelming. You might be worried about what it means for your daily life, your independence, and your future. Here's what we want you to know: while PAD is a serious condition that requires attention, it doesn't have to stop you from living the life you want.
With the right daily habits and lifestyle adjustments, many people with PAD manage their symptoms successfully, slow disease progression, and stay active doing the things they love. Whether you enjoy hiking Colorado's trails, working in your garden, or simply walking around town, a good management plan can help you keep doing those activities.
At Ascent Vascular, we work with PAD patients every day to develop personalized management strategies that fit their lives. This guide will walk you through the practical, day-to-day steps that make the biggest difference in living well with peripheral arterial disease.
Understanding Your New Normal
First, let's set realistic expectations. PAD is a chronic condition, which means it's something you'll manage long-term rather than cure completely. But here's the encouraging part: the daily habits that help manage PAD are the same healthy habits that improve your overall health, reduce your risk of heart attack and stroke, and help you feel better in general.
Think of PAD management as an investment in your future self. The effort you put in today pays dividends in better mobility, fewer symptoms, and reduced risk of serious complications down the road.
The Power of Walking: Your Most Important Tool
If you do nothing else for your PAD, walk. Seriously. A structured walking program is the single most effective lifestyle intervention for peripheral arterial disease. It might seem counterintuitive since walking can cause leg pain, but that's exactly why it works.
Why Walking Helps
When you walk to the point of mild discomfort and then rest, you're actually training your body to develop new, smaller blood vessels (called collateral vessels) that can bypass blocked arteries. Over time, this improves blood flow to your legs and reduces symptoms.
Walking also:
- Strengthens your leg muscles so they use oxygen more efficiently
- Improves your overall cardiovascular health
- Helps control weight, blood pressure, and cholesterol
- Boosts your mood and energy levels
How to Start a Walking Program
Start where you are. If you can only walk for 5 minutes before pain starts, that's your starting point. There's no shame in beginning small.
Follow the "walk until it hurts" approach. Walk at a comfortable pace until you feel leg discomfort (not severe pain, just noticeable discomfort). Then stop and rest until the discomfort goes away, usually 2-5 minutes. Then start walking again. Repeat this cycle for your total exercise time.
Aim for at least 30-45 minutes total (including rest breaks), 3-5 days per week. As your endurance improves, you'll be able to walk longer before needing to rest.
Increase gradually. Each week, try to walk just a bit farther before stopping to rest. Progress might be slow, but any improvement is worth celebrating.
Be consistent. Regular walking is what builds those new blood vessels. Missing weeks sets you back.
Track your progress. Keep a simple log of how far you walked and how long before you needed to rest. Seeing improvement over time is incredibly motivating.
Walking Tips for Colorado's Climate
Living in Edwards means dealing with altitude, changing weather, and winter conditions. Here's how to adapt:
Altitude matters. You might need to start slower than someone at sea level. Give yourself grace as your body adjusts.
Cold weather: Bundle up to keep legs warm. Cold constricts blood vessels, which can worsen PAD symptoms. Layer up and don't skip walks just because it's chilly.
Winter conditions: If ice and snow make outdoor walking unsafe, head to an indoor track, mall, or gym. Safety first.
Summer heat: Walk in the morning or evening when it's cooler. Stay well-hydrated.
If walking outdoors isn't feasible, a treadmill works great. Some people even find it easier to maintain a consistent pace and track their progress on a treadmill.
Daily Foot Care: Non-Negotiable
With PAD, reduced blood flow to your feet means minor injuries can turn into serious problems. A small blister or cut that would heal quickly in someone without PAD might become an ulcer that won't heal. That's why daily foot care isn't optional, it's essential.
Your Daily Foot Check Routine
Every single day, inspect your feet carefully:
Look at the tops, bottoms, and between your toes. Use a mirror or ask someone to help if you have trouble seeing the bottoms of your feet.
Check for:
- Cuts, scrapes, or blisters
- Redness or swelling
- Changes in skin color
- Warm or hot spots
- Calluses or corns
- Ingrown toenails
- Cracks in the skin, especially between toes or on heels
If you notice anything unusual, don't wait to see if it gets better. Contact our team right away. Early treatment prevents minor issues from becoming major problems.
Proper Foot Care Practices
Wash your feet daily with mild soap and lukewarm (never hot) water. Dry them thoroughly, especially between toes where moisture can cause problems.
Moisturize to prevent dry, cracked skin, but skip the areas between your toes where excess moisture invites fungal infections.
Trim toenails carefully. Cut straight across, not too short. If you have trouble seeing or reaching your toes, see a podiatrist for regular nail care.
Never go barefoot, even indoors. Always wear shoes or slippers to protect your feet from injury.
Choose the right footwear:
- Well-fitting shoes that don't pinch or rub
- Soft, breathable materials
- No pointed toes or high heels
- Break in new shoes gradually
- Check inside shoes before putting them on (a small pebble or rough seam can cause blisters)
Wear clean, dry socks that aren't too tight. Avoid socks with thick seams that can cause pressure points.
Don't try to remove calluses or corns yourself. Let a healthcare professional handle these.
Skip the heating pads on your feet. Reduced circulation means reduced sensation, so you might not feel burning until it's too late.
Monitoring Your Symptoms
Living with PAD means staying tuned in to your body. Learning to recognize changes in your symptoms helps you know when to adjust your routine and when to call your doctor.
What to Track
Keep a simple journal or use your phone to note:
Pain patterns: How far can you walk before pain starts? Is it getting better, worse, or staying the same?
Rest pain: Any leg or foot pain when you're resting or sleeping is a red flag that needs immediate medical attention.
Skin changes: New wounds, color changes, or temperature differences between your legs.
Overall function: Can you do the activities you could do last month? Last week?
When to Call Your Doctor
Contact Ascent Vascular right away if you experience:
- Pain in your legs or feet when resting or at night
- Wounds, sores, or ulcers on your feet or legs
- Sudden increase in leg pain
- Changes in skin color (very pale, blue, or dark)
- Legs or feet feeling much colder than usual
- Significant reduction in how far you can walk
- Signs of infection (redness, warmth, swelling, drainage from wounds)
Don't adopt a "wait and see" approach with these symptoms. Early intervention prevents serious complications.
Eating for Better Circulation
What you eat directly affects your PAD. A heart-healthy diet helps slow plaque buildup, improve cholesterol levels, control blood pressure, and manage diabetes if you have it.
Focus on These Foods
Fruits and vegetables: Aim for at least 5 servings daily. They're packed with antioxidants and nutrients that protect your blood vessels. Fresh, frozen, or canned (without added salt or sugar) all count.
Whole grains: Choose whole wheat bread, brown rice, oatmeal, and whole grain pasta instead of refined grains. These help control blood sugar and cholesterol.
Lean proteins: Fish (especially fatty fish like salmon), skinless poultry, beans, lentils, and nuts provide protein without excess saturated fat.
Healthy fats: Olive oil, avocados, nuts, and fatty fish contain fats that actually help your vascular system. Use these instead of butter or margarine.
Water: Stay well-hydrated. Dehydration makes your blood thicker and harder to pump through narrowed arteries.
Limit or Avoid
Saturated and trans fats: Found in fatty meats, full-fat dairy, fried foods, and many processed snacks. These contribute to plaque buildup.
Excess sodium: Too much salt raises blood pressure. Aim for less than 2,300 mg daily (1,500 mg if you have high blood pressure).
Added sugars: Especially important if you have diabetes. Skip sugary drinks, desserts, and processed foods with hidden sugars.
Processed meats: Bacon, sausage, deli meats are high in sodium and saturated fat.
You can learn more about how healthy habits prevent vascular problems on our blog.
Practical Eating Tips
Plan ahead. Having healthy food available makes good choices easier.
Read labels. Check sodium, saturated fat, and added sugar content.
Cook at home more often. You control what goes into your food.
Don't try to overhaul everything at once. Start with one or two changes and build from there.
It's okay to enjoy treats occasionally. Focus on overall patterns, not perfection.
Quitting Smoking: The Most Important Step
If you smoke, quitting is hands-down the most important thing you can do for your PAD. Smoking damages blood vessel walls, reduces oxygen in your blood, accelerates plaque buildup, and increases the risk of blood clots. It also makes PAD symptoms worse and increases your risk of amputation.
We know quitting is incredibly difficult. Nicotine is highly addictive, and if you've been smoking for years, it's a deeply ingrained habit. But it's absolutely worth it.
Why Quitting Helps
Within weeks of quitting, your circulation begins to improve. Within months, your risk of heart attack starts dropping. Long-term, former smokers with PAD have significantly better outcomes than those who continue smoking.
Strategies That Help
Talk to your doctor about smoking cessation aids. Nicotine replacement therapy (patches, gum, lozenges), prescription medications, and counseling all improve your chances of success.
Identify your triggers. What situations make you want to smoke? Develop alternative responses to those triggers.
Get support. Tell friends and family you're quitting and ask for their encouragement. Consider joining a quit-smoking program.
Expect setbacks. Most people try several times before quitting for good. If you slip up, don't give up. Start again.
Replace the habit. When you get a craving, have a plan. Go for a walk, chew gum, call a friend, or do something with your hands.
Your Ascent Vascular team can connect you with resources and support for quitting smoking. It's that important.
Managing Other Health Conditions
PAD rarely exists in isolation. Many people also have diabetes, high blood pressure, high cholesterol, or other conditions. Managing these effectively is crucial for controlling your PAD.
Diabetes Control
If you have diabetes, keeping your blood sugar well-controlled protects your blood vessels from further damage. High blood sugar accelerates PAD progression and increases complications risk.
Check your blood sugar as recommended by your doctor.
Take medications as prescribed.
Follow your meal plan and exercise regularly.
Work closely with your diabetes care team to keep your A1C in target range.
Blood Pressure Management
High blood pressure damages artery walls and accelerates plaque buildup.
Take blood pressure medications exactly as prescribed, even if you feel fine.
Monitor your blood pressure at home if recommended.
Reduce sodium in your diet.
Stay active and maintain a healthy weight.
Cholesterol Control
High cholesterol contributes directly to the plaque blocking your arteries.
Take cholesterol medications (statins or others) as prescribed. Many PAD patients benefit from these medications even if cholesterol levels seem okay.
Eat a low-saturated-fat diet rich in fiber.
Get regular cholesterol checks to ensure medications are working.
Medication Management
Most people with PAD take several medications. Managing them properly is essential.
Common PAD Medications
Antiplatelet drugs (like aspirin or clopidogrel) prevent blood clots. Take these consistently to reduce your risk of heart attack and stroke.
Cholesterol medications (statins) slow plaque buildup and stabilize existing plaque.
Blood pressure medications protect your blood vessels.
Cilostazol might be prescribed specifically to improve walking distance. It can help some people walk farther before experiencing pain.
Diabetes medications if you have diabetes.
Medication Best Practices
Set reminders so you don't miss doses. Phone alarms, pill organizers, or linking medication times to daily routines all help.
Don't skip doses because you feel fine. These medications work to prevent problems, not just treat symptoms.
Never stop medications without talking to your doctor, even if you're experiencing side effects. There might be alternatives or solutions.
Keep an updated medication list with you. Include medication names, doses, and timing.
Ask questions if you're not sure why you're taking something or how it works. Understanding helps with compliance.
Use the same pharmacy for all medications. Pharmacists can catch potential drug interactions.
Staying Active Beyond Walking
While walking is your primary exercise, staying active in other ways benefits your overall health and quality of life.
Safe Activities for PAD
Swimming or water aerobics: Excellent low-impact exercise that's easy on joints.
Cycling: Many people with PAD find they can cycle longer than they can walk because cycling uses muscles differently.
Strength training: Building muscle strength helps with daily activities. Use light weights or resistance bands. Focus on upper body and core when legs are tired.
Stretching and flexibility exercises: Keeps you limber and prevents injury.
Yoga or tai chi: Improves balance, flexibility, and stress management.
Activities to Approach Carefully
Avoid sitting for long periods. Get up and move every hour.
Be cautious with intense exercise that causes severe leg pain. Some discomfort is okay during walking, but severe pain is a signal to stop.
Skip activities with high injury risk to your feet and legs, especially if you have poor sensation.
Talk to your vascular specialist before starting any new exercise program. We can help you choose activities that are safe and beneficial for your specific situation.
Emotional and Mental Health
Living with a chronic condition affects more than your physical health. It's normal to feel frustrated, worried, or even sad sometimes.
Managing the Emotional Side
Acknowledge your feelings. It's okay to have days when PAD gets you down.
Stay connected with friends and family. Social support matters for both physical and mental health.
Focus on what you can do, not what PAD limits. Many people with PAD continue enjoying hobbies, traveling, and staying active.
Celebrate small victories. Walking an extra minute, choosing a healthy meal, or going a day without smoking are all worth recognizing.
Ask for help if you're feeling overwhelmed or depressed. Talk to your doctor about mental health resources.
Join a support group to connect with others who understand what you're dealing with.
Adapting Your Home and Lifestyle
Small changes to your environment can make daily life easier and safer with PAD.
Home Modifications
Keep floors clear of clutter, cords, and rugs that could cause trips and falls.
Install good lighting, especially on stairs and in bathrooms.
Use a shower chair if standing in the shower causes leg pain.
Keep frequently used items at waist level so you don't have to bend or reach excessively.
Consider a grabber tool for picking things up without bending.
Daily Life Adjustments
Plan rest breaks into your day. Don't push through severe fatigue or pain.
Pace yourself. Break tasks into smaller chunks with rest in between.
Ask for help with physically demanding tasks when needed.
Stay warm in cold weather. Keep legs covered and warm to maintain good circulation.
Elevate your legs when resting (but not higher than your heart if you have arterial disease, unless your doctor specifically recommends it).
Planning for Travel
Having PAD doesn't mean you can't travel, but it does require some extra planning.
Before You Go
Talk to your doctor about your travel plans. Get a checkup before extended trips.
Pack all medications in your carry-on with extras in case of delays.
Bring a copy of your medication list and doctor's contact information.
Research medical facilities at your destination just in case.
Get travel insurance that covers medical needs.
During Travel
Move regularly. On long flights or car trips, get up and walk every hour. Do ankle circles and leg stretches in your seat.
Stay hydrated, especially on planes where air is dry.
Wear compression stockings if recommended by your doctor.
Break up long drives with frequent stops to walk around.
Bring comfortable walking shoes and plan activities that allow for rest breaks.
Working with Your Healthcare Team
Managing PAD successfully means maintaining a good partnership with your healthcare providers.
Regular Check-ups
Keep all scheduled appointments, even when you're feeling fine. Regular monitoring helps catch problems early.
Be honest about how well you're following treatment recommendations. Your doctor can't help if they don't know what's really happening.
Report changes in symptoms promptly. Don't wait for your next scheduled visit if something concerning develops.
Get recommended tests like vascular ultrasounds to monitor your condition.
Communication Tips
Prepare for appointments. Bring your symptom log, medication list, and questions.
Take notes during appointments or bring someone who can help you remember what was discussed.
Ask for clarification if you don't understand something.
Discuss treatment goals and whether your current plan is helping you meet them.
At Ascent Vascular, we're partners in your care. We want to hear about your challenges, celebrate your successes, and adjust your treatment plan as needed to help you live your best life with PAD.
Looking at the Long Term
PAD is a marathon, not a sprint. The daily habits you build now will serve you for years to come.
Setting Realistic Goals
Focus on process goals (walk 4 times this week) rather than outcome goals (cure my PAD). You control the process.
Make gradual changes that you can sustain long-term rather than dramatic overhauls that burn you out.
Expect plateaus and setbacks. They're normal. What matters is getting back on track.
Measure success broadly. Better walking distance is great, but so is better cholesterol numbers, successful smoking cessation, or simply feeling more energetic.
Staying Motivated
Remember your why. What do you want to be able to do? See your grandchildren grow up? Keep hiking? Maintain independence?
Track your progress. Seeing improvement, even small amounts, keeps you going.
Reward yourself for meeting goals (just not with unhealthy foods or behaviors).
Connect with others managing PAD. Shared experiences help.
Be kind to yourself. You're managing a chronic condition. That's hard work, and you deserve credit for the effort.
FAQs About Living with PAD
Can I still exercise if walking causes pain?
Yes, and you should. The mild to moderate pain you feel when walking with PAD is actually part of what makes walking therapeutic. Walk until you feel discomfort, rest until it resolves, then walk again. This cycle helps your body develop new blood vessels over time. However, if pain is severe, happens at rest, or is different from your usual claudication, contact your doctor.
How long does it take to see improvement from lifestyle changes?
It varies by person, but many people notice improvements in walking distance within 3-6 months of consistent exercise and lifestyle modifications. Some changes, like better cholesterol levels, might show up on blood tests before you feel physical differences. Stick with it even if progress feels slow.
Should I be taking aspirin for PAD?
Many people with PAD benefit from antiplatelet medications like aspirin, but this decision should be made with your doctor based on your overall health, bleeding risk, and other factors. Never start or stop aspirin without medical guidance.
Can PAD affect both legs equally?
PAD can affect one or both legs, and severity can differ between legs. Some people have symptoms only on one side, while others have bilateral disease. This is something your vascular specialist can assess with physical examination and testing.
Is it safe to get a pedicure with PAD?
Pedicures carry infection risk for people with PAD due to reduced circulation and healing ability. If you choose to get one, go to a reputable salon with proper sterilization procedures, and never allow them to cut cuticles or aggressively remove calluses. Many doctors recommend having a podiatrist handle nail care instead.
What should I do if I develop a blister or cut on my foot?
Clean it gently with mild soap and water, apply antibiotic ointment if recommended by your doctor, and cover it with a clean bandage. Monitor it closely for signs of infection (increasing redness, warmth, swelling, drainage, or red streaks). Contact your doctor right away if it's not healing or shows signs of infection. Don't wait.
Can I still work with PAD?
Many people with PAD continue working successfully. However, jobs requiring prolonged standing or walking might need modifications. Talk to your employer about accommodations like sitting breaks, job restructuring, or assistive devices if needed. Your doctor can provide documentation if necessary.
Will my PAD keep getting worse no matter what I do?
Not necessarily. While PAD is progressive in some people, lifestyle changes and proper medical management can slow or even stabilize the disease in many cases. Some people with mild to moderate PAD maintain stable symptoms for years with good management. The key is being proactive with treatment and lifestyle modifications.
FAQs About Ascent Vascular Specialist and Vein Center
Do you offer supervised exercise programs for PAD patients?
We can provide guidance on starting a walking program and connect you with resources for supervised exercise when appropriate. During your appointments, we'll discuss the best exercise approach for your specific situation and fitness level.
How often will I need follow-up appointments for PAD?
This varies based on your disease severity and how well you're managing. Some patients need visits every 3-6 months, while others with stable, well-controlled PAD might come annually. We'll create a follow-up schedule that's right for you.
Can you help me coordinate care with my other doctors?
Absolutely. We work closely with primary care physicians, endocrinologists, cardiologists, and other specialists to ensure coordinated care. We'll communicate with your other providers and make sure everyone is on the same page with your treatment plan.
What should I do if I have a PAD emergency after hours?
For severe rest pain, sudden onset of cold or numb legs, or wounds showing signs of serious infection, go to the emergency room or call 911. For urgent but non-emergency concerns, call our office at (970) 926-1003 and follow the instructions for after-hours care.
Do you provide nutritional counseling for PAD patients?
We can provide general guidance on heart-healthy eating and connect you with registered dietitians who specialize in cardiovascular nutrition if more detailed counseling would benefit you.
Can PAD treatment improve my symptoms enough that I don't need to change my lifestyle?
Medical and procedural treatments can definitely help improve symptoms, but lifestyle modifications remain important regardless of treatment. Think of treatments and lifestyle changes as working together, not as one replacing the other. The best outcomes come from combining both approaches.
Your Partner in PAD Management
Living well with peripheral arterial disease requires daily attention, but it doesn't require giving up the life you love. With the right strategies, support, and medical care, you can manage your symptoms, slow disease progression, and maintain an active lifestyle.
At Ascent Vascular Specialist and Vein Center, we're here for the long haul. We don't just diagnose and treat PAD, we partner with you in ongoing management. Whether you need help adjusting your exercise program, troubleshooting new symptoms, or exploring additional treatment options, we're here to support you every step of the way.
Ready to take control of your PAD management? Contact us today to schedule an appointment or call our Edwards office at (970) 926-1003. We serve patients throughout the Vail Valley and surrounding Colorado mountain communities.
Visit us at: Ascent Vascular Specialist and Vein Center 1140 Edwards Village Blvd. B204 Edwards, CO 81632
You can also learn more about peripheral arterial disease, explore our treatment options, or read more vascular health information on our blog.
Your journey with PAD doesn't have to be one you walk alone. Let's work together to help you live your best life.
Disclaimer: The information provided on this blog is for general informational purposes only and is not intended as, and should not be considered, medical advice. All information, content, and material available on this blog are for general informational purposes only. Readers are advised to consult with a qualified healthcare professional for medical advice, diagnosis, or treatment. The author and the blog disclaim any liability for the decisions you make based on the information provided. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.